
Being the head of any government agency comes with a myriad of public scrutiny. For Dr. Margaret Chan, her time as Director General of the World Health Organization (WHO) meant the end of a positive public image in the international public health sphere. Elected by secret vote in 2006, she came into her position on the back of praise for her containment of a swine flu and of SARS as a top public health official in Hong Kong.1 Her image was soon dirtied in her response to the H1N1 virus outbreak in 2009, and to the Ebola Virus outbreak in 2014.
The Ebola outbreak of 2014 started in Guinea, Africa in March of that year. This was not immediately abnormal, as there had been periodic outbreaks of the disease, primarily in Africa, since its discovery in 1976. As cases rose, Doctors without Boarders (referred to by their French acronym MSF) began a major response effort. Overwhelmed by the demand and lack of resources, they desperately grasped for the attention of the international community as well as leadership from the WHO.2 Dr. Chan was the head of the WHO, but at that stage, had little control over the relief effort. At the time, the outbreak was mainly combated by the MSF. Within the WHO, it was handled by the organization’s regional operation: AFRO lead by Dr. Sambo.3
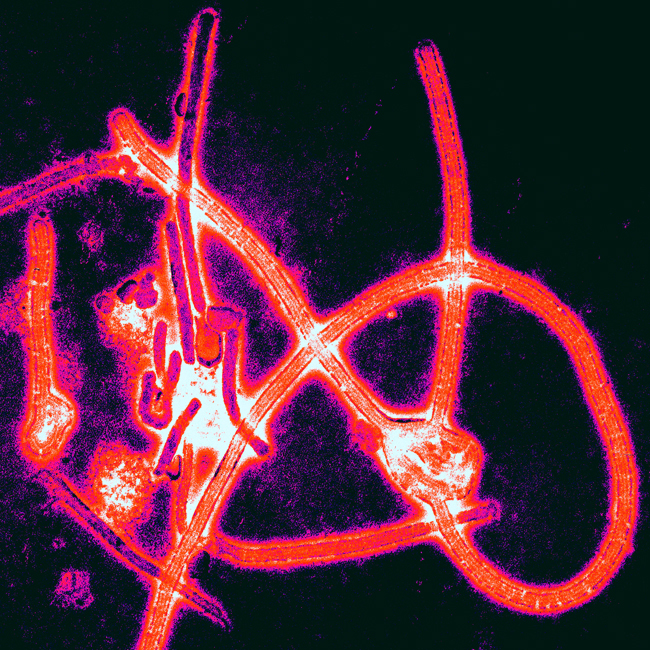
The Ebola Virus Disease, primarily referred to as Ebola or EVD, starts with a common fever and muscle aches, but can progress to gastrointestinal issues and unexplained hemorrhaging. It can be extremely fatal if left untreated or undertreated. It is passed through contact with bodily fluids such as blood or saliva.4 The countries of Guinea, Liberia, and Sierra Leone have extremely fluid boarders and the virus spread between them almost immediately after its discovery. A hot zone at their borders was set up for surveillance shortly after its discovery as a fast-moving disease. While the spread was technically international, it was at first contained well within these three countries. Surveillance of the crisis was ordered by the WHO in April. This lead to a report calling the outbreak the most complex Ebola outbreak in the disease’s history. Continued criticism from the MSF and public calls for leadership got Dr. Chan involved and personally associated with the emergency in June, three months after the discovery of the new strand of the disease.5
Dr. Chan immediately knew she needed to take the outbreak seriously. She promised this to the international community. The greatest power held by the Director General of the WHO is to declare a “public health emergency of international concern” (PHEIC). The WHO has advisory abilities no matter the situation, but their legal power comes solely from scenarios where a PHEIC is declared. This is underwritten in the International Health Regulations (IHR).6 The IHR defines a PHEIC as “an extraordinary event determined… to be a public health risk to other States through the international spread of disease and to potentially require a coordinated international response.”7 The goal during this time was to control the emergency with as little damage to the economic and political climate of the countries as possible. Under this declaration, the WHO can legally enforce quarantine and sanitation requirements. If a UN member state wants to add or shift these regulations to be more thorough, they are legally obligated to inform and get the approval of the WHO. The Director General has more power under this declaration than at any other time. They coordinate relief effort between countries involved and endorse any emergency committees created for the cause.8

Chan’s primary criticism came from her hesitation to order a PHEIC. There were many factors that affected this decision. Chan was placed under an enormous amount of pressure during this time. The systems and circumstances were stacked against her ability to tackle this disease. The road to the declaration was only months long, but it dragged out for the West African people as well as for the international community. The public was unaware of the complexities Chan was facing. For the second time in her career, she was placed at the center of a public health emergency, and was herself under a microscope.
The first time Chan received criticism as General Director was during the H1N1 outbreak in 2009. This influenza outbreak was a terrifying risk to public health at its inception. The illness had spread to 73 countries. Chan released a worried report that a world pandemic had arrived. However, fatalities from the disease turned out to be much lower than expected. Response efforts were left unnecessary, and the tragedy was avoided. Chan was told that she acted in too much of a rush.9 In her effort to take the outbreak seriously, she declared a PHEIC prematurely. This caused fear, distrust, and a waste of resources. Chan went into the Ebola outbreak with this debacle in mind. She wanted to take it seriously, but move forward cautiously. Her first step after taking responsibility for the crisis was to declare it a level three emergency. This is the highest rating before a PHEIC. Her response was primarily diplomatic and related to fundraising. Chan portrayed confidence and seriousness, but the lack of action and result led to continued public scrutiny. Criticism only grew from there.
The first meeting held by Dr. Chan about the relief effort was an urgent high-level ministerial meeting. It hosted a large variety of participants from high-ranking health officials to representatives of airline companies.10 Chan had the complexity of the issue in mind. Her collection of this meeting showed her knowledge that the relief effort would not be straight forward. Challenges continued to pile up. Despite her knowledge of these issues, there was very little she could do.
One of these mentioned challenges was distrust of international officials. This made reporting percentages low. While failure to report to the WHO is technically illegal under IHR guidelines, enforcement mechanisms were ineffective. In addition, there was a lack of databases for previous infections, which made future tracking challenging. There were obvious gaps in the research and reporting, but Chan was helpless in filling these gaps. Challenges in contact tracing proved to be one of the biggest factors to perpetuate the disease. This is true for all infectious diseases, but what shows this in this outbreak was the response in Nigeria. Their more successful contact tracing led to a much lower infection rate.11 This disparity between countries is something that the WHO doesn’t put enough recognition towards.
There was also a risk of social unrest when implementing travel and trade regulations. This is especially true for the countries that were involved because they started with a weak economic infrastructure with recent political instability.12 One goal of implementation of the IHR is to minimize economic effects, but there is no road map to make that happen. Dr. Chan was expected to balance all of these factors. It is an almost impossible task, but Chan forged onward.
Knowing the leadership style that Chan took on as an international official, these social factors were a total nightmare for the doctor. Chan was known for never wanting to isolate any country in their cultural and political beliefs.13 In an attempt to collaborate well with the West African countries involved, she collaborated with community and religious leaders to raise awareness and safety about the disease.14 Much of her initial action, though, was to subvert responsibility away from the WHO and onto the countries themselves. Such a response was representative of her stance as director. She believed that the WHO was an organization to be run by its member states. This was a very different approach from her predecessor, Gro Harlem Brundtland, who is widely remembered in a positive light for his hardline stance and clear leadership. Chan had already received criticism for not being stern about the health of individuals in the LGBTQ community in countries run by theocracies. Her emergency responses have gained similar criticism.15 In this way, Chan’s approach to her position was paradoxical. She was criticized for avoiding criticism.
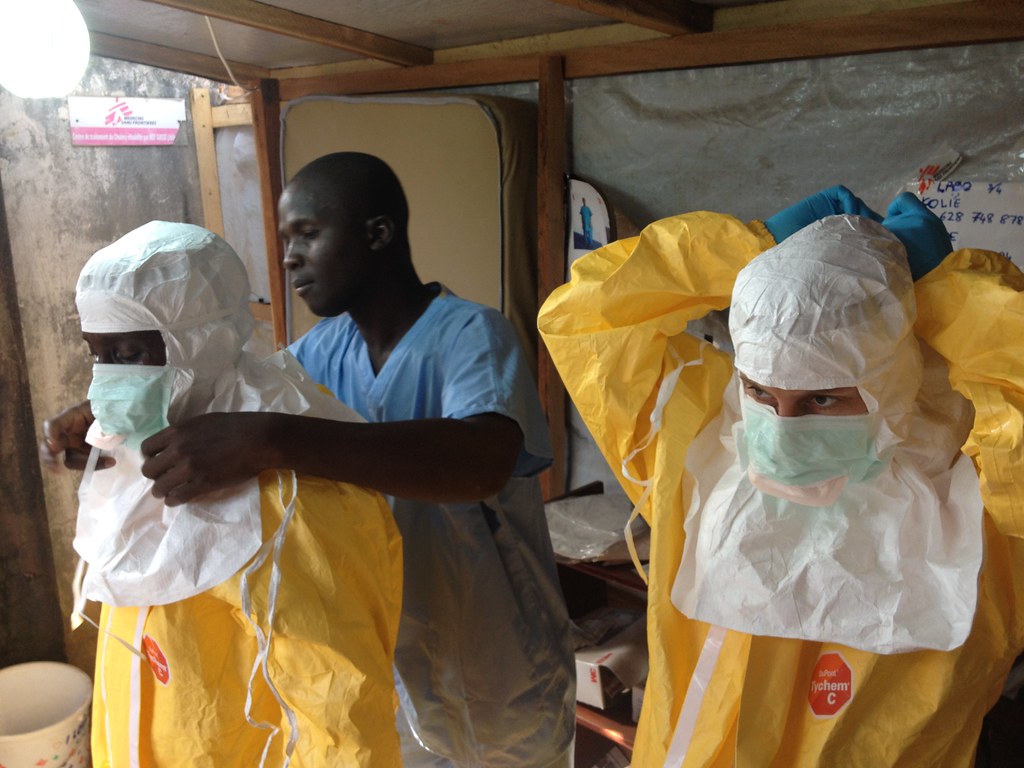
Chan’s next action was to call a conference to secure donors for the response effort. The UN had sent the Global Outbreak Alert and Response Network (GOARN) to help the relief effort, but the WHO was relatively ineffective with their given budget. Chan acknowledged this completely and without reservation. She pointed out that the current resources would leave them with an inability to make a difference in the crisis. Further observation of the virus suggested a third wave of transmission that would spread faster than before.16 With this looming ahead, Chan feared the lack of resources that would soon appear.17 Major funding projects are almost always left with gaps. This adds to the inability of the WHO to make a major difference. In addition to the logistical challenges that they were already facing, Chan didn’t have nearly enough resources to tackle the problem. She knew that disaster would lay ahead.
To address the mounting distress that the west African countries were facing, Chan called a meeting between the leaders of the three most affected countries. She reemphasized the importance of personal responsibility of each respective government. In addition to the talk, the leaders formed a joint resolution, which created an isolation zone regulated by the police and the military.18 Chan and the WHO’s actions here reveal another of the shortcomings of the organization. It assumes equal—or at least a common baseline—power between all of the member states. The IHR defines in articles 5 and 13 that countries must meet a minimum “core public health capacity” by 2012. Only a third of countries were able to meet that requirement.19 Guinea, Sierra Leone and Liberia were three of those countries. The WHO makes a declaration to what countries should do and some have no ability to put that declaration into practice. When Chan placed the response in the hands of these country’s leaders, she neglected to recognize the logistical challenges in doing so. This crisis did not show the failures of Dr. Chan as a person, but the failures of the system she was supposed to work within.

On July 20, the fear that the disease would leave the region was realized.The first case was discovered in Lagos, Nigeria, brought there by a plane traveler, then in Guinea, and in Sierra Leone. It was this case that finally caused Dr. Chan to call a meeting to discuss grounds to declare this situation a PHEIC. Such a meeting is defined in the IHR. A vote is taken to decide the next best steps. 20 Critics are correct in their assessment that this is not when the outbreak became a crisis. By this date, there had already been 1766 cases and 959 deaths.21 The risk of this continued trend was already high and early action could have saved many lives. Yet, the movement they were looking for from the WHO and their director was finally coming.
The meeting took place on August 8, 2014. The committee voted unanimously to declare the crisis a “Public Health Emergency of International Concern.” When asked about this delay later, Chan stated that it could have been moved forward days, but not weeks and certainly not months.22 Two and a half weeks passed between the first confirmed case in Lagos and the declaration. The question to whether the timing was appropriate for the declaration comes down to what the responsibility of the WHO is and what can be done to help countries with limited public health networks. The WHO defends themselves on their website by saying that the declaration was, “neither the start of the WHO response nor the first warning by WHO to the international community about the severity of the situation, both of which had started months before.” They go on to rave about GOARN’s “stern warnings” early on in their response.23 Chan herself said the PHEIC should have been declared only after the spread to Nigeria. Yet, it was this emergency response that made the world lose trust in the WHO. Dr. Chan bears partial responsibility for that legacy.
The outbreak turned out to be devastating in Sierra Leone, Guinea, and Liberia. Where spread outside of these countries had limited devastation, the outbreak was not contained as it could have been. Statistics on the disease are hard to confirm, but there were an estimated 28,000 cases, over 15,000 laboratory confirmed cases, and over 11,000 deaths. In all other affected countries, there were only 34 laboratory confirmed cases and 15 deaths.24 This shows that proper measures can contain the disease more effectively. This raises questions about the role of the WHO and when they need to step in.

Dr. Chan is remembered for doing her best, but also for not implementing effective measures to combat the outbreak. She received a lot of criticism, but she was working within a system that limited her ability to make a difference in the response. She was limited by WHO mechanisms, limitation in resources, lack of legal legitimacy for her role, and a complex network of responses that could not work together effectively. Dr. Chan recognized these challenges, but public opinion did not recognize these challenges as it pertained to Chan’s reputation. Her “head of state pleaser” attitude gained her more criticism and added to the challenges that ended her career. Dr. Chan was not able to overcome the obstacles to providing an effective public health response of international proportion.
- Chan Wai Yin and Ma Shu Yin, “The Making of a Chinese Head of the WHO: A Study of the Media Discourse on Margaret Chan’s Contest for the WHO Director-Generalship and its Implications for the Collective Memory of SARS,” International Journal of Health Services 39, no. 3 (2009): 587-614, http://www.jstor.org/stable/45131157. ↵
- “World Looks for a Better Doctor,” POLITICO (blog), January 22, 2017, https://www.politico.eu/article/world-looks-for-a-better-doctor/. ↵
- N Alexander, “Key Events in the WHO Response,” World Health Organization, 2015, https://www.who.int/news-room/spotlight/one-year-into-the-ebola-epidemic/key-events-in-the-who-response-to-the-ebola-outbreak. ↵
- “Transmission | Ebola Hemorrhagic Fever,” Centers for Disease Control and Prevention, January 14, 2021, https://www.cdc.gov/vhf/ebola/transmission/index.html. ↵
- N. Alexander, “Key Events in the WHO Response,” World Health Organization, 2015, https://www.who.int/news-room/spotlight/one-year-into-the-ebola-epidemic/key-events-in-the-who-response-to-the-ebola-outbreak. ↵
- Robert Frau, “Law as an Antidote: Assessing the Potential of International Health Law Based on the Ebola-Outbreak 2014,” Goettingen Journal of International Law 7 (n.d.): 44. ↵
- Article 1 IHR, 2005 ↵
- Robert Frau, “Law as an Antidote: Assessing the Potential of International Health Law Based on the Ebola-Outbreak 2014,” Goettingen Journal of International Law 7 (n.d.): 44. ↵
- Tsung-Ling Lee, “Making International Health Regulations Work: Lessons from the 2014 Ebola Outbreak,” Vanderbilt Journal of Transnational Law 49 (n.d.): 54. ↵
- N. Alexander, “Key Events in the WHO Response,” World Health Organization, 2015, https://www.who.int/news-room/spotlight/one-year-into-the-ebola-epidemic/key-events-in-the-who-response-to-the-ebola-outbreak. ↵
- Olushayo Oluseun Olu et al., “Contact Tracing during an Outbreak of Ebola Virus Disease in the Western Area Districts of Sierra Leone: Lessons for Future Ebola Outbreak Response,” Frontiers in Public Health 4 (2016): 130, https://doi.org/10.3389/fpubh.2016.00130. ↵
- Tsung-Ling Lee, “Making International Health Regulations Work: Lessons from the 2014 Ebola Outbreak,” Vanderbilt Journal of Transnational Law 49 (n.d.): 54. ↵
- “World Looks for a Better Doctor,” POLITICO (blog), January 22, 2017, https://www.politico.eu/article/world-looks-for-a-better-doctor/. ↵
- N. Alexander, “Key Events in the WHO Response,” World Health Organization, 2015, https://www.who.int/news-room/spotlight/one-year-into-the-ebola-epidemic/key-events-in-the-who-response-to-the-ebola-outbreak. ↵
- “World Looks for a Better Doctor,” POLITICO (blog), January 22, 2017, https://www.politico.eu/article/world-looks-for-a-better-doctor/. ↵
- N. Alexander, “Key Events in the WHO Response,” World Health Organization, 2015, https://www.who.int/news-room/spotlight/one-year-into-the-ebola-epidemic/key-events-in-the-who-response-to-the-ebola-outbreak. ↵
- Tsung-Ling Lee, “Making International Health Regulations Work: Lessons from the 2014 Ebola Outbreak,” Vanderbilt Journal of Transnational Law 49 (n.d.): 54. ↵
- N. Alexander, “Key Events in the WHO Response,” World Health Organization, 2015, https://www.who.int/news-room/spotlight/one-year-into-the-ebola-epidemic/key-events-in-the-who-response-to-the-ebola-outbreak. ↵
- Tsung-Ling Lee, “Making International Health Regulations Work: Lessons from the 2014 Ebola Outbreak,” Vanderbilt Journal of Transnational Law 49 (n.d.): 54. ↵
- Robert Frau, “Law as an Antidote: Assessing the Potential of International Health Law Based on the Ebola-Outbreak 2014,” Goettingen Journal of International Law 7 (n.d.): 44. ↵
- “Outbreaks | Ebola Hemorrhagic Fever,” Centers for Disease Control and Prevention, January 14, 2021, https://www.cdc.gov/vhf/ebola/transmission/index.html. ↵
- “World Looks for a Better Doctor,” POLITICO (blog), January 22, 2017, https://www.politico.eu/article/world-looks-for-a-better-doctor/. ↵
- N. Alexander, “Key Events in the WHO Response,” World Health Organization, 2015, https://www.who.int/news-room/spotlight/one-year-into-the-ebola-epidemic/key-events-in-the-who-response-to-the-ebola-outbreak. ↵
- “Outbreaks | Ebola Hemorrhagic Fever,” Centers for Disease Control and Prevention, January 14, 2021, https://www.cdc.gov/vhf/ebola/transmission/index.html. ↵




26 comments
Xavier Bohorquez
Congratulations on winning an Award on this topic. Reading the diverse voices that are represented in this field shows how far we have come from the past. The work which you provided and the contributions you mentioned show how difficult the field of international relations while nations were dealing with a deadly virus is astounding, thanks for sharing Chan’s story where most other news outlets overlooked her contributions.
Emilee Luera
In my perspective, this is a well-written post. I knew little about Ebola save that it was significantly more limited than Covid. At the time, I had no idea who she was, but I had heard her name. Looking back, it appears that she struggled to make the decisions she made during this outbreak, especially considering how everyone responded to the WHO’s information during covid. I’m not saying they were wrong, but I was shocked that people weren’t more worried about Ebola.
Maya Naik
Hello Anna, I want to extend my congratulations on your nomination for Best in Humanities. Your recognition is well deserved. Your article is exceptionally well written and provides informative insights on the challenges of being in a position of influence, particularly in the political arena. It is admirable how you handle the scrutiny that comes with such roles. Keep up the excellent work.
Joseph Frausto
Congratulations on your win. Seeing diverse voices represented in this field where they historically not is very enlightening and shows how far we have come. The work which she contributed to the difficult field of international relations while nations were dealing with a deadly virus is astounding, thanks for sharing Chan’s story where most other news outlets overlooked her contributions. Great job!
Analyssa Garcia
Hi Anna,
Congratulations on your award nomination for Best in Humanities! It is well deserved. I think this article was very well written and is very informative. It sheds a light on the fishbowl you are in whenever you decide to be in important roles like these, especially in political roles. People watch your every move and are waiting to criticize. Great work.
Illeana Molina
Hi Anna, Congrats on your nomination as I know the research, analysis, and gathering of information was not easy. Ebola is incredibly scary as we have seen such as Covid as it was very brand new with little to no information. In times like this, we see communities virtually come together and the WHO and administrations come together to help those around them. Medical health care workers were incredibly strong during this time and I will forever thank them. Great Job and Congratulations
Carollann Serafin
I forgot about Ebola once Covid-19 hit. It is crazy to think how that small pandemic affected us but since it never went beyond widespread to my understanding like Covid-19 I never thought higher officials would take into account the amount of damage it was causing to the world. This article was very interesting and informative
Aaron Astudillo
Hey Anna, I first wanted to congratulate you on the nomination. I recall the global scare that happened when Ebola was gaining global attention, and the deadly outcome that could happen if one where to catch this virus. However, I did not take into much consideration the administrative side and the impact that WHO had on containing the virus.
Vincent Villanueva
Hi Anna, I just wanted to say what a nicely written article! Ebola is such a scary topic to cover just because of how dangerous this outbreak was. It was definitely something we should recognize for international health precautions, especially after the covid-19 pandemic. It was a beautifully written article Anna! Congratulations!
Jared Sherer
Ebola is scary, but politics are hell. Dr. Chan lived with both and her reputation suffered for it. The WHO was set up in a way that prevented Dr. Chan from being effective and timely doing anything about the outbreaks. This is very sad and truly devastating to history. Dr. Chan could only do so much and was not as successful in dealing with the deadly diseases as she knew was necessary. This must have been very frustrating for her. I would like to further research Dr. Chan and what she has done lately. Very well done and thoroughly researched.